C-Reactive Protein CRP Test
C-reactive protein CRP is a protein made in the liver that researchers track as a general inflammation marker, since inflammation can reflect many lifestyle and aging factors. Like elevated homocysteine, a high CRP level increases one’s vulnerability to cardiovascular disease, Alzheimer’s, and cancer, but those connections are best seen as part of broader wellness awareness rather than a specific disease prediction. Such an increase in CRP levels may be caused by infection, inflammation, trauma, diabetes, as well as certain medicines. In the absence of these main factors, elevated CRP can correspond with a higher future risk of heart attack.
This article was last reviewed on 10 April 2019. This article was last modified on 14 February 2020.
In addition, increased systemic inflammation is a sign of aging. Therefore, C-reactive protein (CRP) can be classified as a marker of healthy aging1.
It has been found that this marker predicts well the risk of developing age-related diseases and human life span2.
What is the difference between CRP and hs-CRP?
As you’ve no doubt guessed, the difference between CRP and hs-CRP is contained in the “hs” abbreviation – “high sensitivity.”
RELATED ARTICLES
Traditionally, CRP, or C-reactive protein, is measured down to concentrations of 3 to 5 mg/L; hs-CRP is measured down to concentrations of approximately 0.3 mg/L. This improved sensitivity allows hs-CRP to be used to detect low levels of chronic inflammation.
Researchers explore hs-CRP in wellness studies, and readers can use those findings as background when they talk with their clinician about what their numbers may mean.
Which level is considered the norm?
Concentrations less than 1 mg/L indicate low risk of cardiovascular disease.
1 to 2,9 mg/L levels suggest average risk. Concentrations above 3.0 mg/L indicate a high risk of cardiovascular disease
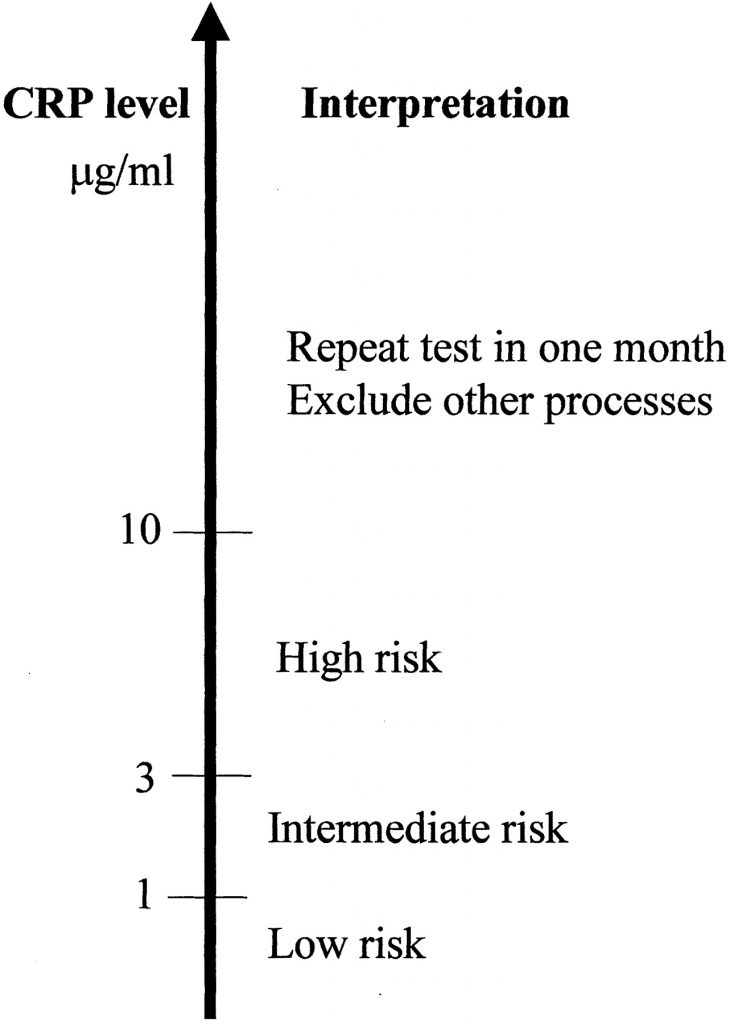
Typical hs-CRP readings reflect broad wellness patterns: lower values generally align with less systemic inflammation, mid-range values are common in everyday living, and readings approaching or above 3.0 mg/L can be a cue to re-engage with your clinician. Only a healthcare professional should interpret these lab results and decide whether any follow-up or repeat testing is appropriate.
As you can see, a reading above 10 mg/L may signal a need for further testing to determine the cause of such significant inflammation in your body. It’s worth mentioning that levels of hs-CRP less than 10 mg/L are significant for cardiovascular risk stratification. Higher hs-CRP levels may be the sign of acute inflammation, a chronic illness, a trauma, etc.
C-Reactive Protein as a Biomarker of Cardiovascular Disease
Public health bodies have investigated hs-CRP alongside traditional markers to better understand inflammation’s role in heart health34.
As for primary prevention, a number of prospective epidemiological studies have shown that the high-sensitivity method in detecting CRP is highly predictive of cardiovascular accidents5, peripheral vascular diseases, ischaemic strokes, and sudden cardiac death risks even if the patient is virtually healthy. Other major studies in the USA and Europe have proven hs-CRP levels to be a better risk indicator than low-density lipoprotein cholesterol levels. Moreover, since hs-CRP reflects a different cardiovascular risk component, research suggests hs-CRP and lipid levels together can inform conversations about heart health. Use these results with your healthcare provider to understand next steps.
» Wondering why you should calculate your biological age? These 5 reasons will convince you to do it now.
Do I need to check my hs-CRP levels if I feel well?
Factors that increase hs-CRP levels are quite numerous. They include obesity, elevated blood pressure, diabetes mellitus type 1 and 2, acute situational reaction, sleep disturbances, etc. Healsens offers educational guidance to help you learn about factors that can influence hs‑CRP and how often people may choose to check it, in consultation with their healthcare provider.
Follow us on Facebook|| Instagram || Telegram || Youtube
What if my C reactive protein CRP level is high?
As we wrote above, for hs-CRP values exceeding 10 mg / L, it is recommended to undergo additional testing to find the causes of inflammation. Since such high levels of hs-CRP are associated with acute inflammation, chronic disease, trauma, etc.
For values below 10 mg / L, the good news is that giving up smoking, regular physical activity, as well as weight-reducing treatment, can lower basic hs-CRP level without any medical help. Healthy eating habits6, green tea78, controlled drinking, sufficient vitamin D910, vitamin C11, and vitamin K12 in your body can also reduce the level of the reactive protein in the body.
In addition, glucosamine may reduce cancer mortality by lowering C-reactive protein levels. Some studies have explored glucosamine’s potential effects on inflammation markers; consult your clinician before considering supplements. This is due to a decrease in inflammation, which will be reflected in a decrease in the inflammatory marker C-reactive protein, as expected by about 23%.
The same effect can be achieved through certain medications, such as13:
- cyclooxygenase inhibitors(Aspirin, Rofecoxib, Celecoxib)
- thrombocyte aggregation inhibitors (Clopidogrel, Abciximab)
- cholesterol management products (statins, ezetimibe, fenofibrate, nicotinic acid)
- beta-adrenergic blocking agents and angiotensin
- converting-enzyme inhibitors (Ramipril, Captopril, Fozinopril)
- anti-diabetes drugs (Rosiglitazone, Pioglitazone).
In case any medications must be taken, discuss your therapeutic regimen with your doctor.
» Discover everything about what your cholesterol results mean.
Ordering Blood Tests in the Netherlands
If you’d like to learn your hs-CRP level, we can point you to third-party laboratories that offer this test; always review options with a healthcare professional.
1. Download the Healsens app from Google Play or the App Store, depending on your device.
2. Complete the registration process in the app.
3. Explore the app’s educational section to find information about common blood tests and how to discuss them with your doctor.
4. Find the hs-CRP test and tap on the “Add to Cart” button. Proceed with the ordering process.
» Unlock Optimal Health: Discover How a Personalized Healsens General Check-up Plan Can Transform Your Well-being.
Note
If you want to assess your hs-CRP level but are not residing in the Netherlands or have opted for a different laboratory, you can record your lab values in the app to track your wellness goals; for medical decisions or result interpretation, please rely on your clinician. Furthermore, you gain full access to investigate your health risk assessment based on the provided data.
FURTHER READING
Source: ©️2019 Healsens B.V. All right reserved
Follow us on Facebook|| Instagram || Telegram || Twitter || Youtube
Source: ©️2019 Healsens B.V. All right reserve
- Association of 10-Year C-Reactive Protein Trajectories With Markers of Healthy Aging: Findings From the English Longitudinal Study of Aging
- Interleukin-6 and C-reactive protein, successful aging, and mortality: the PolSenior study
- High-sensitivity C-reactive protein as a biomarker of risk in coronary artery disease
- 2019 Guidelines on Dyslipidaemias (Management of)
- High-Sensitivity C-Reactive Protein and Cardiovascular Disease Across Countries and Ethnicities
- Diet quality inversely associated with C-reactive protein levels in urban, low-income African American and White adults
- Green tea extract reduces blood pressure, inflammatory biomarkers, and oxidative stress and improves parameters associated with insulin resistance in obese, hypertensive patient
- Green Tea minimally affects Biomarkers of Inflammation in Obese Subjects with Metabolic Syndrome
- Interaction of Vitamin D and Smoking on Inflammatory Markers in the Urban Elderly
- Effect of Vitamin D Supplementation on the Level of Circulating High-Sensitivity C-Reactive Protein: A Meta-Analysis of Randomized Controlled Trials
- A Meta-analysis of Randomized Control Trials: The Impact of Vitamin C Supplementation on Serum CRP and Serum hs-CRP Concentrations
- Relationship between vitamin K status, bone mineral density, and hs-CRP in young Korean women
- C-reactive protein (CRP)-lowering agents

