Type 2 Diabetes: Causes, Diet, Treatments

After posting the publication about lipid profile assessment, we received many comments and questions. Among all the questions, type 2 diabetes and the ineffectiveness of drug treatment were mentioned most often. Therefore, today we will pay attention to this particular topic, dwelling on the following points:
This article was last reviewed by Svetlana Baloban, Healsens, on March 04, 2020. This article was last modified on 15 February 2020.
- Talk about what causes diabetes and focus on the role of nutrition for people suffering from this disease
- Consider different ways of evaluating your lifestyle to find out what may lead preservation, and in some cases, to the progression of this disease
- Try to find an answer to the questions: Why taking drugs may not solve the problem and what are some other ways you can help yourself.
- Cholesterol is in normal ranges having high triglycerides, let’s review possible reasons
- Analyze the psychological aspect of the problem, the role of chronic stress, and ways of handling it
So, diabetes is a condition that affects blood sugar levels and causes many serious health problems if left untreated or uncontrolled. There is no cure for diabetes so that is why it’s easier to head off disease before it occurs than to treat it. Regular health checkups with your clinician can help you stay informed about your overall wellbeing. In case you’ve already got this disease, common approaches your healthcare provider may discuss include nutrition, activity, and other physician-directed options. Other effective medications include non-Sulfonylurea secretagogues, thiazolidinediones, alpha glucosidase inhibitors, and insulin.
Causes of Diabetes Type 2
Genetics and Lifestyle Choices Play a Role
Type 2 diabetes has several causes: genetics and lifestyle are the most important ones. A combination of these factors can cause insulin resistance, when your body doesn’t use insulin as well as it should. Insulin resistance is the most common cause of type 2 diabetes.
IN THIS ARTICLE
RELATED ARTICLES
Genetics and Type 2 Diabetes
Type 2 diabetes can be hereditary. That doesn’t mean that if your mother or father has (or had) type 2 diabetes, you’re guaranteed to develop it; instead, it means that you have a greater chance of developing type 2. Discuss your personal risk for diabetes with a healthcare professional during routine checkups. As for the genetic tests,, despite the fact that researchers know that you can inherit a risk for type 2 diabetes, they haven’t found out which genes carry the risk. The medical community is hard at work trying to figure out the certain genetic mutations that lead to a risk of type 2
Lifestyle Is Very Important
Genes do play a role in type 2 diabetes, but lifestyle choices are also important. You can, for example, have a genetic mutation that may make you susceptible to type 2, but if you take good care of your body, you may not develop diabetes. Moreover, routine wellness lab work, ordered by your clinician, can offer insights into how your body handles nutrients.
If you already suffer from this disease, you have probably heard a lot from the doctor or in the press about the dangers of products containing refined carbohydrates and “white” carbohydrates with the high glycemic index, such as white bread, ground rice, pasta made from premium flour and features potatoes. We will also dwell on this issue in detail and below it will be clear why this issue is so important.
When people eat food containing carbohydrates, the digestive system breaks down the digestible ones into sugar, which enters the blood. As blood sugar levels rise, the pancreas produces insulin, a hormone that prompts cells to absorb blood sugar for energy or storage. As cells absorb blood sugar, levels in the bloodstream begin to fall. When this happens, the pancreas starts making glucagon, a hormone that signals the liver to start releasing stored sugar. This interplay of insulin and glucagon ensure that cells throughout the body, and especially in the brain, have a steady supply of blood sugar.
» Tired and overwhelmed? Check your allostatic load — the science of stress impact.
What happens when you consume too much sugar?
A high sugar diet consumption provokes an instant increase in insulin levels, which sometimes leads to a sharp drop in blood sugar after a few hours. Hypoglycemia caused in this way (low blood sugar) provokes the desire to eat more food rich in refined sugars and starches, which leads to a new jump in insulin.
Over time, these constant “ups and downs” cause cells to lose their sensitivity to insulin, and more and more of this hormone is required for glucose transfer. This is called insulin resistance. And it becomes the root cause of the development of the metabolic syndrome leading to high blood pressure. Likewise, insulin resistance increases the risk of developing coronary heart disease. It’s also accelerating the aging process and can also lead to type II diabetes. With this type of diabetes, the pancreas can become so depleted that it completely stops producing insulin to lower blood sugar. In addition, insulin resistance is a cause of impaired fat metabolism, leading to an excess of triglycerides. That’s why having high triglycerides — a type of fat in the blood — may be a sign that you have prediabetes or type 2 diabetes.
Dietary habits and diabetes

The issue of diet is very acute! However, everyone who tried to give up refined sugar and starches knows how difficult it is and there is a completely rational explanation for this.
In 2001, a study was published in the journal Nutrition Review showing that refined sugars and starches are addictive. And if you want to exclude them from the diet, it can cause withdrawal symptoms. But getting rid of simple carbohydrates in the diet is the only and most important step that should be taken to reduce the risk of getting sick with metabolic syndrome and type 2 diabetes, as well as to reduce body weight if necessary. Only rejection of these products will make this unhealthy habit disappear. Therefore, if you want to just reduce sugar consumption, it will not bring about the elimination of this addiction. A low-glycemic, whole-foods approach is one of several lifestyle habits that support balanced energy and complement clinician-led care for people at risk of metabolic conditions. We’re talking about the Mediterranean diet and DASH Diet.
Glycemic Index and Glycemic Load
The second important point about carbohydrates is that not all of them are harmful. To explain how different kinds of carbohydrate-rich foods directly affect blood sugar, the glycemic index was developed and is considered a better way of categorizing carbohydrates, especially starchy foods. The idea and main focus are to avoid foods with a high glycemic load (you can find tables with lists of products indicating their glycemic index and glycemic load).
The glycemic index indicates how rapidly a carbohydrate is digested and released as glucose (sugar) into the blood stream. In other words, it shows how quickly foods break down into sugar in your bloodstream. A food with a high GI raises blood sugar more than a food with a medium to low GI but does not take into account the amount of carbohydrate in a food. So glycemic load is an indicator of how a carbohydrate food will affect blood sugar. Try to record your diet for a week and check which of the consumed foods are among high-glycemic foods.
Fact
Foods with a low glycemic index have a rating of 55 or less.
Foods with a medium glycemic index range from 56 to 69.
Foods with a high glycemic index are rated 70 to 100.
Measuring Blood Sugar Levels throughout the Day
Some people choose to check their glucose regularly in coordination with their healthcare provider. Such measurement is carried out:
- In the morning, immediately after waking up and before eating
- Before each meal, to answer the following questions:
- How does choosing food and serving size affect my blood glucose?
- When injecting food (short / ultra-short) insulin, it is necessary to check whether the dose of this insulin given before the previous meal was adequate.
- How to adjust the nutrition and serving size in the future?
- Two hours after a meal. We answer the following questions:
- Has your blood glucose returned to your target after eating?
- When injecting dietary (short / ultra-short) insulin, it is necessary to check whether the dose of this insulin given before meals was adequate?
- Before physical activity:
- Do I need to eat before physical activity?
- Is it possible to engage in physical activity or should it be postponed?
- During and after physical activity:
- How has physical activity affect your blood glucose?
- Does physical activity have a delayed effect on blood glucose?
- Is there hypoglycemia?
Examples of how people track their glucose with their care team; always follow personal targets set by your clinician.
| Target Levels by Type | Upon waking | Before meals (pre prandial) | At least 90 minutes after meals (post prandial) |
| Non-diabetic* | 4.0 to 5.9 mmol/L (72 – 106.3 mg/dL) | under 7.8 mmol/L (140.54 mg/dL) | |
| Type 2 diabetes | 4 to 7 mmol/L (72 – 126.13 mg/dL) | under 8.5 mmol/L (153.15 mg/dL) | |
| Type 1 diabetes | 5 to 7 mmol/L (90.09 mg/dL – 126.13 mg/dL) | 4 to 7 mmol/L (72 – 126.13 mg/dL) | 5 to 9 mmol/L (90.09 mg/dL – 162.16 mg/dL) |
| Children w/ type 1 diabetes | 4 to 7 mmol/L (72 mg/dl – 126.13 mg/dL) | 4 to 7 mmol/L (72 – 126.13 mg/dL) | 5 to 9 mmol/L (90.09 mg/dL – 162.16 mg/dL) |
*The non-diabetic figures are provided for information but are not part of NICE guidelines.
When you finish your blood glucose check, write down your results. Then you need to note what factors may have affected them. They might include food, activity, or stress. Take a close look at your blood glucose record to see if your level is too high or too low several days in a row at about the same time. If the same thing keeps happening, it might be time to change your diabetes care plan.
A goal of such medical check up
Work with your care team to shape nutrition and activity choices that support your overall health.
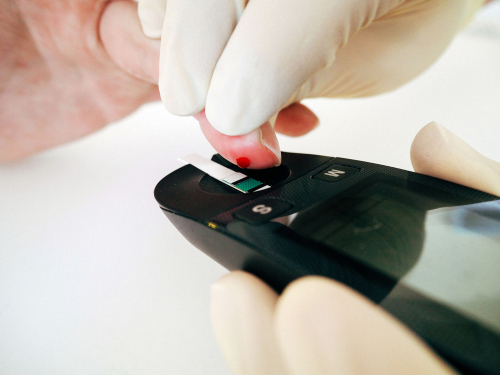
You need to take into account that there may be hidden sugars. It’s especially important for ready-made food in supermarkets. For such cases, this control will make it clear whether the food you are used to buying needs to stay on the shop shelf next time.
Follow us on Facebook|| Instagram || Telegram || Youtube
Continuous Glucose Monitor
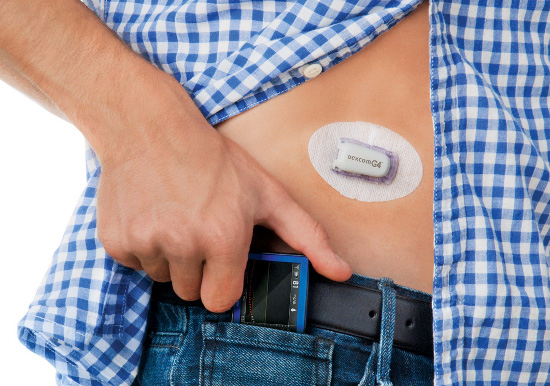
Learn how clinicians explain continuous glucose monitors so you can better understand the technology and its role in formal diabetes care, keeping the focus on informed conversations with your medical team.
Diet changing and physical activity increasing will necessarily lead to weight loss if there is such a problem. And for people with type 2 diabetes, losing at least some weight is a very important factor. Even a little more physical activity can have a positive effect. For example, if you get used to walking more often. So, walking was the most common activity, with numerous studies demonstrating its beneficial effects on reducing the risk of T2 diabetes, cardiovascular diseases, and mortality. Walking for at least 30 min per day was shown to reduce the risk of T2 diabetes by approximately 50%1.
Psychosomatic Aspects Of Type 2 Diabetes
Physical and mental health are very closely related. Moreover, and either can have a significant impact on the other. According to Britneff and Winkley (2013), there is an association between mental health problems and increased diabetes complications. In addition, people with diabetes type 2 run a poorer quality of life. So managing emotional health cannot be less important than keeping blood sugar under control.
Health problems can occur if the stress response goes on for too long or becomes chronic, such as when the source of stress is constant, or if the response continues after the danger has subsided. In addition, chronic stress may also go unnoticed for a long time. That happens because different people may feel stress in different ways. For example, some people experience mainly digestive symptoms. On the other hand, others people may have headaches, sleeplessness, sadness, anger or irritability. People under chronic stress are prone to more frequent and severe viral infections, such as the flu or common cold.
Routine stress may be the hardest type of stress to notice at first. Because the source of stress tends to be more constant than in cases of acute or traumatic stress, the body gets no clear signal to return to normal functioning. In psychology, a constant high blood sugar level is sometimes associated with a resistance. The biological meaning is to help an individual better defend himself with a high sugar level. It means that nature provides additional energy in the form of sugar.
If you feel internal conflicts, experience chronic or routine stress, then in addition to the above recommendations, it is highly desirable taking practical steps to manage your stress.

How to Cope with Stress
The following are some tips that may help you to cope with stress:
- Recognize the Signs of your body’s response to stress. For example, difficulty sleeping, increased alcohol and other substance use, being easily angered, feeling depressed (or use Online Depression Screening), and having low energy.
- Get Regular Exercise. Just 30 minutes per day of walking can help boost your mood and reduce stress.
- Try a Relaxing Activity. Explore stress coping programs, which may incorporate meditation, yoga, tai chi, or other gentle exercises. For some stress-related conditions, these approaches are used in addition to other forms of treatment.
- Set Goals and Priorities. Decide what must get done and what can wait. And learn to say no to new tasks if they are putting you into overload. Note what you have accomplished at the end of the day, not what you have been unable to do.
- Stay Connected with people who can provide emotional and other support. To reduce stress, ask for help from friends, family, and community or religious organizations.
- Schedule a psychologist consultation to mitigate the problems.
Furthermore, numerous studies with non-diabetic populations have shown that performing various positive psychological exercises (e.g., writing gratitude letters, performing acts of kindness) have led to greater well-being2.
In Healsens, you have access to multiple tools for maintaining your mental health and managing stress more effectively. We recommend installing the app and choosing a comprehensive approach, which includes:
✦ Thayer Journals – to record your daily subjective well-being and detect short-term changes in mood and energy.
✦ Beck Journals – to track long-term changes in your mental health status.
✦ Cortisol/DHEA-S and Allostatic Load – Healsens supports stress awareness with journaling templates and reflections so you can bring qualitative notes to your next clinician check-in about how you are feeling.
This integrated approach combines self-observation, biological markers, and professional insights to help you prevent the long-term negative effects of chronic stress and support overall well-being.
Comprehensive Approach to the Management of Diabetes
So, let’s summarize everything we talked about above. To cope with the problem, you need to take a comprehensive approach to assess your nutrition, physical activity, medication, and psychological health. And if the selection and dosage of medications should be carried out without fail by your attending physician, then you can handle the rest yourself.
- Diet Revision
- Exclusion from the diet of foods with a high glycemic load. Maintaining a balance of 33–40% of carbohydrates of the total calorie intake. However, in some cases, it may be necessary to limit the intake of carbohydrates to reduce weight and allow the cells of the pancreas to rest (from several months to a year or more).
- Avoid cereals and fruit juices, drinks.
- Avoid processed meats, especially sausages, sausages, etc.
- Choose fruits with a low glycemic load.
- Eat a moderate amount of legumes (peas, beans, lentils, peanuts, etc.) and nuts (walnuts, cashews, almonds, etc.).
- Increase your intake of low-starch vegetables on the ground, such as white cabbage, cauliflower, Brussels sprouts, leafy cabbage, curly and Beijing cabbage, broccoli, mustard leaves, chard, spinach, lettuce, peppers of all colors, green peas, celery, zucchini, cucumbers, etc. d., raw or after minimal heat treatment.
- Be sure to eat redfish 2-3 times a week.
- Make sure that the amount of incoming salt is moderate.
- Increased physical activity.
- Stress reduction.
If you feel called to share more detailed notes with your healthcare team, keep a simple wellness log of how you feel before and after meals and discuss the patterns rather than suggesting self-directed blood sugar testing.
Thank you for your attention and we hope that the material has been useful to you!
FURTHER READING
Source: ©️2019 Healsens B.V. All right reserved





Like!! Really appreciate you sharing this blog post.Really thank you! Keep writing.
It’ѕ awesome designed for me to have a web page, whіⅽh is valuable for
my know-how. thanks admin
Hola! I’ve been following your blog for a long time now and finally got the bravery to
go ahead and give you a shout out from New Caney Tx!
Just wanted to tell you keep up the excellent job!