Do you know that nearly half of adults in the United States (108 million, or 45%) have hypertension and 22.4% of adults with hypertension are unaware of their condition?1 How about other countries? Globally, 3.5 billion adults now have non-optimal systolic BP levels (that is, >110–115 mmHg) and 874 million adults have systolic BP ≥140 mmHg2. Thus, approximately one in four adults has hypertension. However, studies show that high blood pressure is not an inevitable consequence of aging34. Later on, we will tell you about these studies in detail. In the meantime, let’s talk about what hypertension is and how it can be prevented.
This article was last reviewed by Svetlana Baloban, Healsens,, 2020. This article was last modified on December 14, 2020.
What is Hypertension?
Hypertension is another name for high blood pressure. In 2017, the American College of Cardiology and the American Heart Association published new guidelines for treating hypertension, defining high hypertension as blood pressure at the level of 130/80 mmHg. Stage 2 hypertension is defined as blood pressure of 140/90 mmHg or higher.
This condition can lead to serious health complications and increase the risk of heart disease, stroke, and sometimes death. About two-thirds of adults with hypertension or taking medication to lower blood pressure at the age of 30 have a roughly 40% higher risk of developing cardiovascular disease than their peers.
In addition, cardiovascular disease in people with hypertension appears about 5 years earlier. Managing blood pressure is an important part of general wellness and can support overall longevity.
RELATED ARTICLES
Hypertension Causes
Defining hypertension we need to distinguish between primary and secondary hypertension. The majority of patients suffer from primary hypertension, which is approximately 85% to 95% of all cases. It should be said that the causes of hypertension include several types of genetic issues combined with many factors, which will be discussed below. In almost all of these cases, the disease is associated with a family history. As for secondary hypertension, it accounts for 5% to 15% of all cases. Secondary hypertension means that high blood pressure is caused by another medical condition. For example, high blood pressure can be the result of diseases such as kidney, glandular, and heart disease.
Primary Hypertension
So, speaking of primary hypertension, we primarily talk about genetic predisposition along with many lifestyle factors. What are the most significant factors? First, it is a high sodium (Na+) intake56. Thus, high serum Na+ concentration promotes fluid (water) retention, thereby increasing blood volume and BP. When dietary Na+ increases in normotensive individuals, compensatory haemodynamic changes occur to maintain constant BP. These changes include a decrease in renal and peripheral vascular resistance and an increase in nitric oxide production by the endothelium. However, if the action of nitric oxide is impaired or absent, an increase in blood pressure occurs.
The second factor is poor sleep quality or sleep apnea. Also, excessive alcohol consumption and high mental stress contribute to the development of hypertension.
Finally, the likelihood of developing hypertension increases with age due to progressive hardening of the arterial vasculature. This induration is caused, among other things, by slowly developing changes in vascular collagen and an increase in atherosclerosis7. Finally, immunological factors can also play an important role. So, against the background of infectious or rheumatological diseases, such as rheumatoid arthritis, hypertension may develop.8
Follow us on Facebook|| Instagram || Telegram || Youtube
Secondary Hypertension
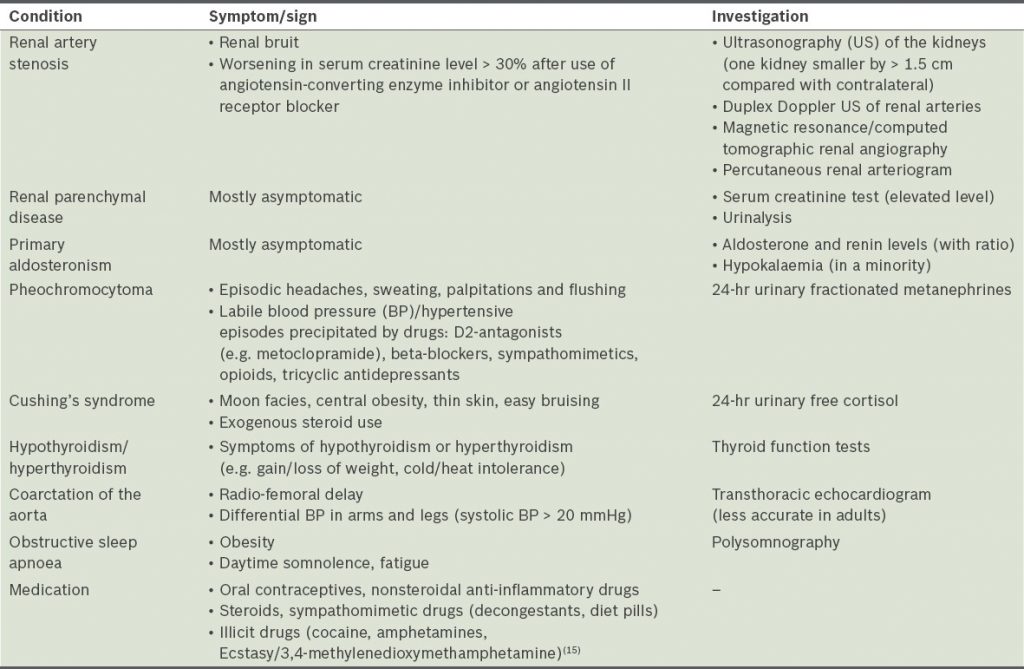
As we mentioned above, secondary hypertension means that it is caused by some other medical condition. Let’s talk about important clues pointing to some other causes of hypertension. First of all, such clues include young age. So, in young people under 30 years of age, renal causes or coarctation of the aorta (narrowing of the aortic lumen) are often determined. And it is because of these problems that the pressure rises. It is also helpful to understand what symptoms or signs may indicate secondary causes of high blood pressure (see table 1).
Very high readings or pressures that stay elevated despite multiple lifestyle or care approaches should prompt a conversation with a healthcare professional. Much attention should be paid to a sharp exacerbation of hypertension in a patient with previously stable control.
Diagnosis of Hypertension
High blood pressure is a silent danger, because only a few patients have clear hypertension symptoms. Thus, it’s important to know what hypertension is. Periodically noting how your blood pressure feels can keep you mindful of overall well-being and lifestyle trends9. We are talking about such conditions as white coat hypertension (isolated clinical hypertension) and masked (isolated outpatient) hypertension.
How to measure your blood pressure?
Consistent, relaxed self-checks can help you observe how your body responds to daily habits; track small variations to notice when you might want to revisit your routine.
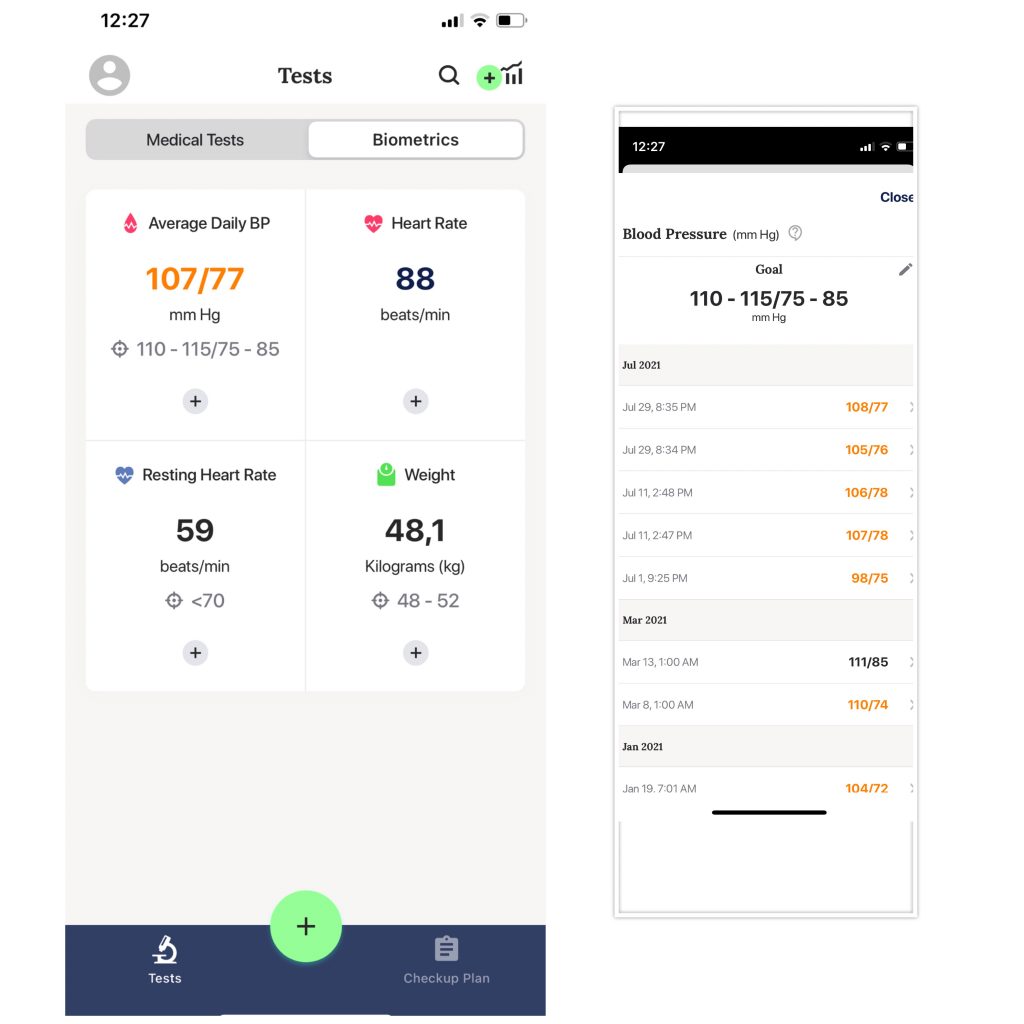
“The Healsens app can help you capture and reflect on your blood-pressure trends so you stay aware of how daily habits affect you.”
If you notice any deviations, then it makes sense to measure your blood pressure twice in the morning and twice in the evening for at least 3 days, and preferably 7 days. After that, calculate the average for all measurements for the last 2 days to 6 days, depending on the measurements made for 3 or 7 days, respectively. As a rule, the readings of the first day are skipped. When taking morning and evening measurements, pay attention to the following recommendations.
- Blood pressure is measured in the morning 30 minutes after waking up, but before taking medication or having breakfast.
- Blood pressure is measured in the evening before taking medication.
Follow us on Facebook|| Instagram || Telegram || Youtube
What is normal blood pressure?
The American College of Cardiology and the American Heart Association have released their updated guidelines for blood pressure (Table 2)10.
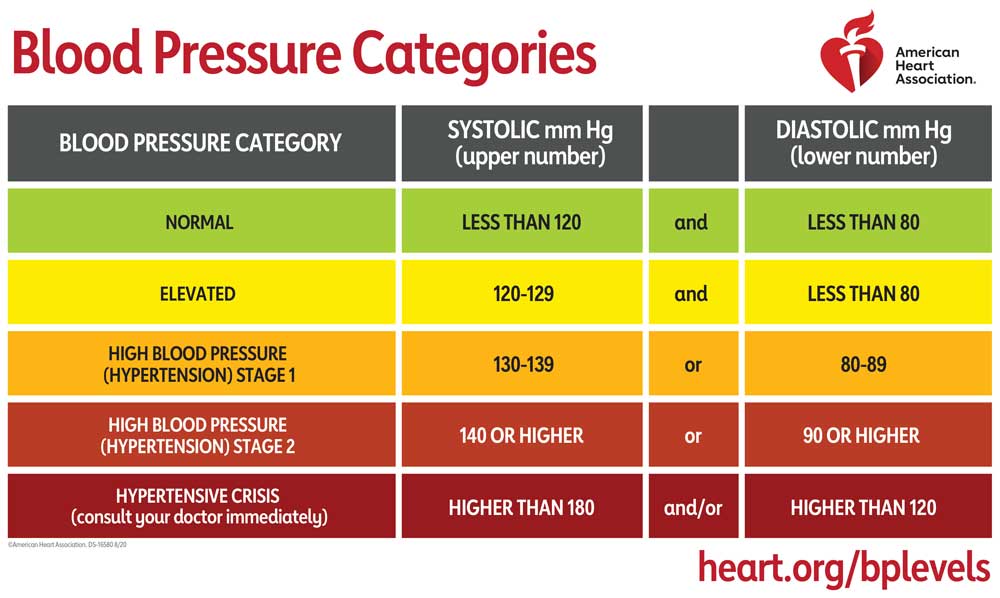
As you can see, high blood pressure (without a diagnosis of hypertension) is systolic blood pressure between 120 and 129. Previously, this was an undefined category called “prehypertension.” As we wrote above, measurements must be obtained from at least two exact measurements in two different cases.
Laboratory investigations in the diagnosis of hypertension
The very fact of an increase in pressure is only a small part of the necessary examinations. It was mentioned before, a small proportion of patients have a potentially reversible cause of hypertension. This means that for such people, a correct diagnosis can lead to a cure or a significant improvement in blood pressure control. Therefore, it is advisable to perform simple screening for secondary hypertension in all patients (Box 1).
It is also worth paying attention to whether there were any manifestations of hypertension in the anamnesis. For example, hypertension may have been observed during pregnancy, which is an important factor in evaluating women with hypertension. Thus, medical history is very important in assessing the risk of cardiovascular disease. You can revisit popular calculators to reflect on how lifestyle choices may influence heart-health trends as part of your general wellness habits.
“The app offers general wellness calculators to help you reflect on heart-health factors; only medical professionals can provide clinical risk assessments.”
“Follow us for general wellness tips and app updates that help you track healthy habits.”
Box 1 – Laboratory investigations in the diagnosis of hypertension
Routine tests:
1. Haemoglobin and haematocrit
2. Fasting plasma glucose
3. Serum total cholesterol, low-density lipoprotein cholesterol, high-density lipoprotein cholesterol
4. Fasting serum triglycerides
5. Serum potassium and sodium
6. Serum uric acid
7. Serum creatinine
8. Estimated glomerular filtration rate (eGFR)
9. Urine analysis including a test for microalbuminuria
10. 12-lead EKG
Specialized evaluations are handled by healthcare providers; your role is to share your readings and concerns with them.
FURTHER READING
Source: ©️2019 Healsens B.V. All right reserved
Follow us on Facebook|| Instagram || Telegram || Twitter || Youtube
Source: ©️2019 Healsens B.V. All right reserve
- Facts About Hypertension
- Global Burden of Hypertension and Systolic Blood Pressure of at Least 110 to 115 mm Hg, 1990-2015
- Migration, blood pressure pattern, and hypertension: the Yi Migrant Study
- The Kenyan Luo migration study: observations on the initiation of a rise in blood pressure
- Sodium in Your Diet
- Hypertension
- Vascular Aging and Arterial Stiffness
- Hypertension
- Methodology and technology for peripheral and central blood pressure and blood pressure variability measurement: current status and future directions – Position statement of the European Society of Hypertension Working Group on blood pressure monitoring and cardiovascular variability
- Monitoring Your Blood Pressure at Home

