High Homocysteine Levels: 5 Strong Reasons to Pay Attention

High homocysteine levels are being studied in relation to overall wellness and aging. Talk to your doctor about any concerns. Homocysteine is an amino acid normally produced in the body during the metabolism of methionine, an essential amino acid found in protein-rich foods. Ideally, its levels in the blood should remain low, as excess homocysteine is toxic and can damage the lining of blood vessels, contributing to heart attacks, strokes, Alzheimer’s disease, depression, and osteoporosis.
Although homocysteine testing is rarely included in routine check-ups, growing research highlights its central role in aging, metabolic imbalances, cognitive impairment, and even infertility. Below, we’ll explore five key reasons why it’s important to monitor and manage high homocysteine levels.
5 Reasons to Pay Attention to Homocysteine Levels
1. High homocysteine has been associated in research with cardiovascular health challenges
High homocysteine levels can damage the inner lining of blood vessels, making them fragile and more prone to injury. Cholesterol and calcium can then deposit on these damaged areas, forming plaques. This process triggers inflammation and activates the blood clotting system, raising the risk of atherosclerosis, blood clots, heart attacks, and strokes1.
2. It’s dangerous during pregnancy
During pregnancy, maintaining balanced nutrition, including folate, supports healthy development.
3. Research explores how homocysteine relates to general vascular wellness.
Homocysteine increases oxidative stress and promotes chronic inflammation in blood vessels. This accelerates vascular aging, reduces arterial elasticity, raises blood pressure, and contributes to the development of cardiovascular complications.
RELATED ARTICLES
4. Some studies examine homocysteine in relation to cognitive wellness.
High homocysteine levels have been associated with brain atrophy and cognitive decline — especially in older adults. This may be due to deficiencies in B vitamins (particularly B6, B12, and folate), which are essential for proper homocysteine metabolism. When these vitamins are lacking, brain energy levels drop, inflammation increases, and neural function becomes impaired.
5. Elevated homocysteine is being researched alongside mood and brain health.
Research suggests that high homocysteine levels can play a role in the development of psychiatric conditions, including depression and even schizophrenia. One possible mechanism involves overstimulation of NMDA receptors in the brain, leading to oxidative stress and inflammation. People with elevated homocysteine often report symptoms such as irritability, anxiety, poor memory, and sleep disturbances.
What Are the Symptoms of High Homocysteine Levels?
High homocysteine levels often go unnoticed — which makes them particularly dangerous. There may be no obvious signs for years, even as the damage accumulates silently in blood vessels, brain tissue, and bones. When symptoms do appear, they’re often mistaken for age-related changes, chronic stress, or vitamin deficiencies.
According to a 2023 StatPearls review (NCBI Bookshelf), high homocysteine levels may be associated with the following symptoms and conditions:
- Chronic fatigue
- Numbness or tingling in the limbs
- Memory issues and cognitive impairment
- Unexplained weight loss
- Depression
- Schizophrenia
- Dementia (including Alzheimer’s disease)
- Increased risk of hip fractures
- Osteoporosis
- Chronic kidney disease
- Hypothyroidism
If you experience any of these symptoms — especially in combination — you can discuss homocysteine testing with a healthcare professional if you’re curious about your wellness markers.
» Tired and overwhelmed? Check your allostatic load — the science of stress impact.
How Often Should You Check Your Homocysteine Levels?
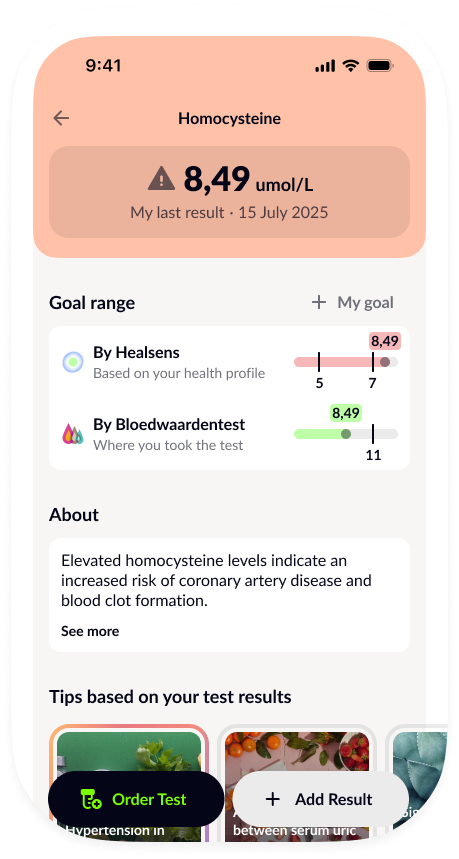
The frequency of checking your homocysteine levels depends on your individual risk factors. At Healsens, this test is often recommended alongside a vitamin B12 assessment, since B12 deficiency is one of the most common causes of impaired homocysteine metabolism.
Among Healsens users, we regularly observe high homocysteine levels not only in older adults, but also in younger individuals — starting from age 26 and up. Elevated levels are especially common in people with B12 deficiency, chronic stress, low animal protein intake, or genetic variations affecting methylation pathways.
You should consider testing your homocysteine levels if you have:
- A family history of stroke, heart attack, thrombosis, or coronary artery disease
- Blood clotting disorders
- Neurological development issues in children
- Preparation for pregnancy or IVF
- Pregnancy complications or fetal birth defects
- Smoking habits
- Regular alcohol consumption
- Symptoms of depression
- Age over 75
Even if you don’t fall into these categories, a homocysteine test may still be valuable — especially if you have low B12 levels, an elevated biological age, or any of the symptoms mentioned earlier.
If the test shows high homocysteine levels, retesting is typically recommended after 3–6 months, following dietary adjustments, supplement use, or other lifestyle changes.
Some estimates suggest that reducing homocysteine levels by just 40% could extend life expectancy by 8 years per 1,000 men and 4 years per 1,000 women. That makes this simple blood test a powerful tool for prevention and longevity.
» Discover everything about what your cholesterol results mean.
Which level of Homocysteine passes for normal?
The “ideal” homocysteine level levels of about 5-7 µmol/L2.
“Good” levels of less than 10 µmol/L3. So, homocysteine > 10 μmol/L is associated with some risk factors like peripheral microvascular endothelial dysfunction (PMED), higher major cardiovascular events, etc.
The normal range of homocysteine levels are less than 15 micromoles per liter (mcmol/L).
Higher levels are: Moderate (15 to 30 mcmol/L); Intermediate (30 to 100 mcmol/L); Severe (greater than 100 µmol/L).
Any higher than 15 and you will want to consider discussing your results with a healthcare professional.
The latest studies show that homocysteine is an independent risk factor of cardiovascular diseases4. Clinical research shows that a 5 umol/L elevation in homocysteine concentration in blood plasma increases the vulnerability to cardiovascular disease and total mortality by 1.3 – 1.7 times. Some studies explore whether lifestyle changes influencing homocysteine relate to heart health; evidence is evolving.
If levels of homocysteine are found to be elevated, it is advisable to measure the levels of creatinine, thyroid stimulating hormones, folacin, cobalamine to define probable causes of hyperhomocisteinemia and suggest appropriate treatment.
Follow us on Facebook|| Instagram || Telegram || Youtube
How to explore homocysteine information within the Healsens app.
Information about homocysteine blood tests is provided for discussion with your healthcare provider.
Living in the Netherlands, Belgium, or Germany? You can easily check your homocysteine levels using the Healsens app — right from your phone.
💡 The homocysteine test is not included in the standard Vitality Check: 21 package. However, if you share certain wellness inputs, the app may suggest educational content about homocysteine. You can also order it anytime via the test catalog.
Here’s how to order the test:
1. Download the Healsens app from the Google Play or the App Store, depending on your device.
2. Register in the app to unlock personalized features.
3. Go to “Browse Tests” and search for the homocysteine test.
4. Tap “Add to Cart” and complete your order.
» You can log your lab values to see trends alongside general lifestyle tips; clinical interpretation should come from your clinician.
Note
Not in the Netherlands, Belgium, or Germany, or using a different lab? No problem — you can have the recommended blood tests done at any local lab.
Then, manually enter your results in the Healsens app. Based on your data, you’ll receive:
✦ General lifestyle suggestions are provided for educational purposes; consult a healthcare professional for medical advice.
✦ General wellness insights based on the information you enter.
✦ personalized insights and follow-up guidance
Healsens remains your personal guide to preventive health — no matter where you are.
Causes for High Homocysteine Levels
At first, don’t panic if your homocysteine level is above the norm values.
Just because you have high homocysteine doesn’t mean you will develop heart disease or a neurological condition tomorrow, next week or even next month.
Track wellness patterns over time and consult clinicians for any concerns. And if you’re already dealing with a chronic disease, then by examining your homocysteine levels, you’ve gotten one big step closer to uncovering the root cause and getting your health back on track.
It’s worth mentioning that smokers are more vulnerable to hyperhomocysteinemia. Moreover, high coffee consumption is one of the most powerful factors increasing homocysteine in blood. Those who drink more than six cups of coffee a day have 2-3 umol/L higher homocysteine levels than people who drink no coffee.
Elevated homocysteine levels are often associated with a sedentary lifestyle. So, moderate physical activity lowers homocysteine levels in case of hyperhomocysteinemia. Vegan diet can also decrease its levels by 13% without any supplements.
However, the most frequent cause of high homocysteine levels is folacin deficit5. The deficit of cobalamine (vitamin В12) may also lead to homocysteine accumulation6. However, the effectiveness of using vitamins is a subject of debate among researchers. Several major randomized experiments showed that relatively easy lowering of homocysteine levels through taking supplements did not result in lowering vulnerability to cardiovascular diseases7.
FURTHER READING
Source: ©️2019 Healsens B.V. All right reserved
Follow us on Facebook|| Instagram || Telegram || Twitter || Youtube
Source: ©️2019 Healsens B.V. All right reserve
- Hyperhomocysteinemia
- Homocysteine: Friend or Foe?
- Elevated plasma homocysteine levels are associated with impaired peripheral microvascular vasomotor response
- Homocystein–an independent risk factor for cardiovascular and thrombotic diseases
- Folic Acid Deficiency
- Vitamin B12 and homocysteine
- Homocysteine‐lowering interventions for preventing cardiovascular events




